HSCI researchers develop a more accurate model of human skin with fat, nerves, and hair
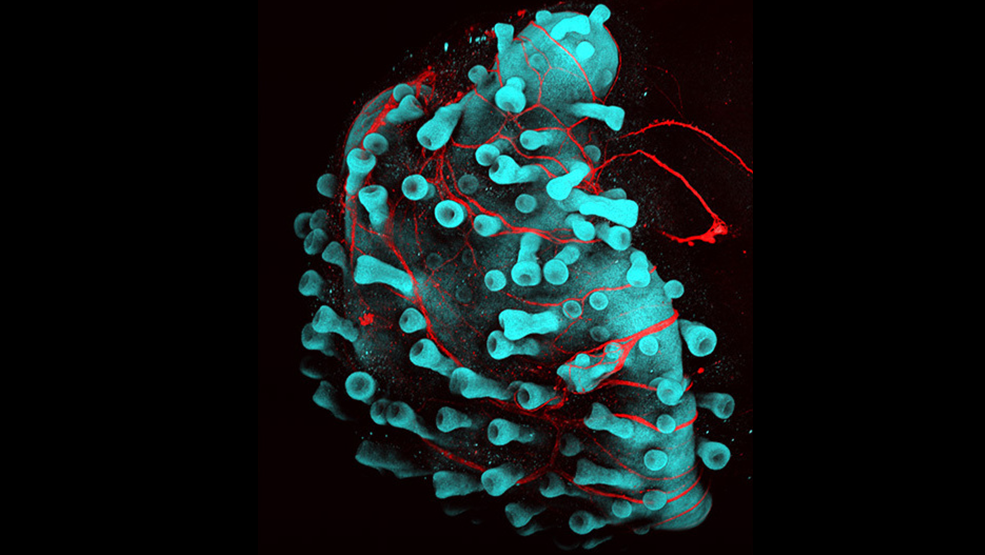
For more than 40 years, scientists have been recreating human skin in the lab. Yet all of these models have lacked many of the component cells and structures of normal skin, including hair.
Now, HSCI researchers have cultured human skin cells that are capable of growing hair and are embedded with fat and nerves in a multi-layer structure. The achievement represents more than five years of work led by Karl Koehler, whose lab was originally at the Indiana University School of Medicine and is now at Boston Children’s Hospital. The technique is published in the journal Nature.
“In this latest work, we discovered a way to grow both layers of human skin together,” Koehler said, referring to the top epidermis layer and bottom dermis layer. “Those cells talk to each other in a skin organoid culture — or skin in a dish we created — and sprout hair follicles accompanied by fat and nerve cells.”
Taking the results a step further, the team transplanted the human hairy skin into mice. The mice developed human hair follicles at the site of transplantation. Potential uses for the new technique will include testing drugs as well as treating burns, healing wounds, and other therapeutic applications.
Growing skin in a dish
Previously in 2018, the researchers showed that they could generate hairy skin from mouse stem cells. Here, to create the human equivalent, the team started with human induced pluripotent stem cells.
“We applied a cocktail of growth factors and small molecules, kind of a cooking recipe for human pluripotent stem cells,” Koehler said.
When culturing the skin organoids in a dish, the team first noticed co-development of the epidermis and dermis. The interactions and signaling between the two tissue layers led to budding of hair follicles at 70 days, which corresponded with the timing of hair development in the human fetus.
“It is amazing that the timing of normal skin development is so well preserved in the dish,” said Jiyoon Lee, lead author the study and research associate in the Koehler lab.
In addition to growing hair, the organoids produced fat and muscle-like cells of the skin, as well as nerves similar to those that mediate touch sensation.
“The fat is an unsung hero of the skin and recent studies suggest it plays a critical role in wound healing,” Lee said.
The organoids also produced Merkel cells, specialized touch-responsive cells of the skin that have been implicated in diseases such as Merkel cell carcinoma.
“The inclusion of these other cell types likely expands the potential uses of the skin organoid model to research on sensory disorders and cancer,” she added.
Transplanting skin organoids
To test the skin organoids, the researchers cultured the organoids for over four months and then implanted them on the backs of mice.
“We noticed that within a month, tiny brown hairs sprang up from the transplant site,” Lee said. “This showed us, amazingly, that pigment cells also developed in the organoids.”
They compared the transplanted skin with adult human skin samples, observing several unique features of human skin in the transplants. One included ‘rete ridges,’ or valleys in the wavy pattern of human epidermis that helps anchor it into skin membranes. Furthermore, the transplanted hair developed elaborate sebaceous glands that produced sebum, the natural oil that lubricates human skin.
A proof of concept
Translating any mouse study into humans is a long road. “But we think we have developed a proof of concept showing that the cells integrate into skin and form outgrowing hair follicles,” Koehler said.
The researchers hope they can use the technology to seed wound beds with cultured skin to reconstruct skin, in cases such as extensive burns or scars. And while it might be tempting to think of the approach as a potential “cure” for baldness, Koehler cautioned that many challenges lay ahead.
“We now have a technique that could generate nearly unlimited hair follicles for transplantation,” he said. “But immune rejection is a major hurdle, and generating follicles tailored to an individual will be incredibly costly and take a year or more.”
To meet these challenges, the researchers are working on ways to speed up the timeline of growth in a dish, as well as how to engineer organoids to evade immune detection or make them efficiently from patient-derived cells.
Read more
This story was originally published on the Boston Children’s Hospital website on June 10, 2020.
Lee, J. (2020). Hair-bearing human skin generated entirely from pluripotent stem cells. Nature. DOI: 10.1038/s41586-020-2352-3
This research was supported by the National Institute of Arthritis and Musculoskeletal and Skin Diseases, the Ralph W. and Grace M. Showalter Trust, the Indiana Clinical and Translational Sciences Institute, and the Indiana Center for Biomedical Innovation.
