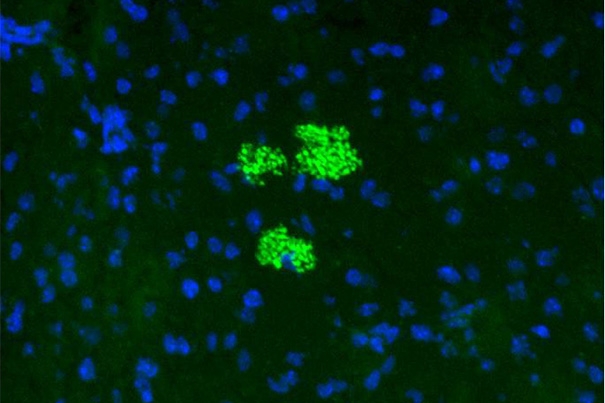
Mesenchymal stem cells (green) colonize a pancreatic islet in a preclinical model of diabetes. The blue dots represent the nuclei of cells within the islet.
by Haley Bridger, Brigham and Women's Hospital Communications
Researchers at Harvard-affiliated Brigham and Women’s Hospital (BWH) studying mesenchymal stem cells (MSCs) — a cell type useful in treating immune-related diseases — have uncovered a way to enhance and prolong the cells’ therapeutic effects in a preclinical model of type 1 diabetes.
The research team, led by Harvard Medical School (HMS) Professor Robert Sackstein of BWH’s Departments of Dermatology and of Medicine and HMS Associate Professor Reza Abdi of BWH’s Department of Medicine and Transplantation Research Center, reports its results this week in the journal Stem Cells.
In type 1 diabetes, the body’s immune cells obliterate pancreatic islets, where insulin is produced. MSCs are a type of adult stem cell with potent immune-suppressing and anti-inflammatory effects. In preclinical trials using diabetic-prone mice (non-obese diabetic mice), researchers had previously found that intravenous administration of MSCs could dampen pancreatic injury by reducing the levels of sugar in the mice’s bloodstreams without insulin administration, but these effects were modest and temporary.
Sackstein and his team hypothesized that if more MSCs could be forced to populate inside the pancreatic islets, more islets could be spared from immune destruction, yielding a more complete reversal of diabetes.
MSCs normally lack a key cell surface adhesion molecule called HCELL, which mediates the homing of cells in the bloodstream to sites of tissue inflammation. The injection of MSCs directly into pancreatic islets is not feasible because the pancreas is fragile and releases highly toxic enzymes when manipulated. To get intravenously administered MSCs to the sites of the immune attack, the research team engineered the HCELL homing molecule to steer them toward the inflamed pancreatic islets.
The team found that administering HCELL-bearing MSCs into diabetic mice caused the MSCs to lodge in the islets. The result was durable normalization of blood sugar levels, eliminating the need for insulin administration — a sustained reversal of diabetes
Sackstein, co-corresponding author of the study, concluded that while further studies of the effects of MSCs are warranted, the preclinical study represents an important step in the potential use of mesenchymal stem cells in the treatment of type 1 diabetes and other immune-related diseases.
