
By Nancy Fleisler (Boston Children's Hospital) and Javier Barbuzano (Harvard Stem Cell Institute)
To stay healthy, our lungs have to maintain two key populations of cells: the alveolar epithelial cells, which make up the little sacs where gas exchange takes place, and bronchiolar epithelial cells (also known as airway cells) that are lined with smooth muscle.
“We asked, how does a stem cell know whether it wants to make an airway or an alveolar cell?” says Carla Kim, PhD, of the Stem Cell Research Program at Boston Children’s Hospital, and Executive Committee member of the Harvard Stem Cell Institute.
Figuring this out could help in developing new treatments for such lung disorders as asthma and emphysema, manipulating the natural system for treatment purposes.
It’s been widely assumed that epithelial stem cells direct the formation of these two cell types, but the picture turns out to be more complicated.
To investigate lung-cell formation, Kim and Joo-Hyeon Lee, PhD (now at the Cambridge Stem Cell Institute in the U.K.) used a 3D “organoid” culture system they established in 2014. This allowed them to observe what kinds of cells were being made.
To this, they added single-cell RNA sequencing to see what genes each cell type turns on. This enabled Kim and colleagues to identify what the cells are saying to each other.
As reported today in Cell, they found that lung cells known as mesenchymal cells (not to be confused with mesenchymal stem cells) are the cells driving the action. Through the single-cell RNA sequencing, they further found that mesenchymal cells come in at least five flavors, with different molecular signatures.
“All of these cell types are interacting with each other to repair and regenerate lung tissue,” says Kim. “What we learned is that mesenchymal cells are telling the epithelial stem cells what type of lung cell they should make.”
Cells with a marker called LGR5 secrete a lot of a molecule called Wnt5A that promotes the formation of alveolar cells, Kim’s team showed, while cells with the LGR6 marker are important for repair of airway cells.
“If you have a disease like emphysema or bronchopulmonary dysplasia where alveolar cells are not being repaired, stimulating the WNT pathway could be important,” says Kim. “When WNT is blocked, you get the alternate kind of cell. But if you add WNT back in, it goes back to usual.”
For airway problems like asthma, blocking WNT or finding a way to boost the formation of LGR6-bearing cells could be approaches to explore to increase production of airway cells. “We found that if you injure mouse lungs so airway cells are killed off, you need LGR6+ cells to repair that kind of damage,” Kim says.
But she acknowledges that there’s much more to be learned.
“What we really want to know next is, what are all the secreted factors these cells make that can control cell fate? Those could be potential therapeutic targets.”
Joo-Hyeon Lee, PhD, now at the Wellcome Trust, was the study’s first author. The work was supported by the Wellcome Trust and the Royal Society (107633/Z/15/Z), the European Research Council (679411), the Cambridge Stem Cell Institute (07922/Z/11/Z), the American Lung Association (400553), the National Institutes of Health (R01 HL090136, R01 HL132266, R01 HL125821, U01 HL100402 RFA- HL-09-004), the Harvard Stem Cell Institute, the Howard Hughes Medical Institute, the Klarman Cell Observatory and the National Cancer Institute (1U24CA180922, P30-CA14051).
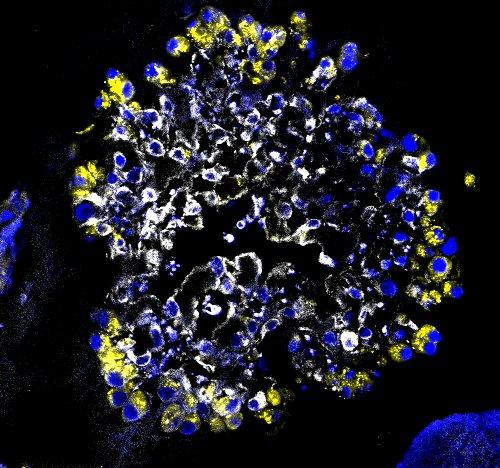
IMAGE CAPTION
Driving lung cell formation: The lung must maintain two key cell populations: bronchiolar cells, also known as airway cells (left), and alveolar epithelial cells, where gas exchange takes place (right). A new study eavesdrops on the crosstalk that determines which cell types are made. Credit: Joo-Hyeon Lee (Boston Children’s Hospital/Cambridge Stem Cell Institute UK)
